Matabeleland South is happy with the change Health Resilience Funds is bringing
on May 8, 2024 in Health and Wellbeing, News, Women and Maternal Health
Health Resilience Fund strengthens access to primary health care in the most remote places in Zimbabwe

In Matabeleland South Province, the Health Resilience Fund is changing access to primary health care services. We saw many happy faces during a recent media field mission to Gwanda, Umzingwane, and Bulilima Districts with the Ministry of Health and Child Care and the Health Resilience Fund Communication Officer. Local communities expressed gratitude for the strengthened healthcare delivery system, which makes basic essential healthcare services available to all, including those in the most remote areas of the Country.
The Health Resilience Fund is a coordinated effort by the Zimbabwean Government and development and technical partners supporting the Ministry of Health and Child Care in attaining Universal Health Coverage for the people of Zimbabwe.
The Fund is led by the Ministry of Health and Child Care and benefits from financial contributions from the European Union, the Governments of Ireland, the United Kingdom, Gavi, the Vaccine Alliance, and technical support from UNFPA, UNICEF, and the WHO.
The programmes supported by the Health Resilience Fund are implemented by the Ministry of Health and Child Care at national, provincial, district and community levels and by implementing partners.

The Health Resilience Fund is about bringing health care close to the people. In the Plumtree District Hospital, a student nurse aide consults a local patient to provide her with the most accurate health services.
The Health Resilience Fund supports the Plumtree District Hospital by training healthcare workers, providing clinical mentorship for doctor-nurse teams, and providing health supplies and medicines.
It functions as a referral hospital for the local health facilities in the area.
Through the support provided at the hospitals and health facilities at the national, provincial, district and local regional levels, the Health Resilience Fund aims to reduce maternal, neonatal and child mortality and teenage pregnancies and to strengthen health systems to tackle current and future health challenges.

The Health Resilience Fund focuses on women, neonates, children under 5, adolescents, youth, and vulnerable populations, including people with disabilities and marginalised populations.
Particular attention goes to the health of adolescent girls, as Zimbabwe faces high levels of early pregnancies.
The Adolescent Pregnancies in Zimbabwe, published recently by the Ministry of Health and Child Care and UNICEF with the support of UNFPA and UNESCO, indicates an adolescent pregnancy prevalence rate in Zimbabwe of 23.7 per cent.
At Plumtree District Hospital, 29 out of the 34 mothers seen at the maternity waiting home on the visit’s day were adolescents under 19.

The nurse in charge of one of the health facilities in Umzingwane District proudly showed her pharmacy.
Thanks to the support of the Health Resilience Fund, drug shortages have become rare in her facility. Accessing essential medicines is key to the Health Resilience Fund’s ultimate objective.
This accessibility contributes to ensuring Universal Health Coverage for all Zimbabweans, meaning everyone in Zimbabwe has access to a full range of quality health services without financial hardship.

Ensuring Universal Health Coverage implies health services are brought to the people, like here through an outreach activity in Matabeleland South.
To end preventable deaths in maternal, newborn and child health, interventions of the Health Resilience Fund emphasise increased availability, equity and access to essential reproductive maternal, new-born, child and adolescent health and nutrition services, including through promoting community participation and bringing health services as close as possible to the people’s everyday environment.

It took us more than two hours driving from Bulawayo, primarily over dirt roads, to reach one of the outreach activities set up by the District Health Office in a remote area of Gwanda District.
Various health interventions were offered to the local communities with the support of the Health Resilience Fund.
Interventions included routine vaccination, vitamin A supplementation and growth control for children, family planning, a wide range of outpatients’ department services, postnatal care (PNC), HIV testing, counselling and treatment, eye-testing, COVID 19 self-testing, visual inspection with acetic acid and camera (VIAC) to prevent cervical cancer in women aged 30-50 years old, and drugs distribution.
The outreach activities mobilised a large group of people across all age groups from the surrounding communities, most of whom do not have any other opportunity to access essential health services.
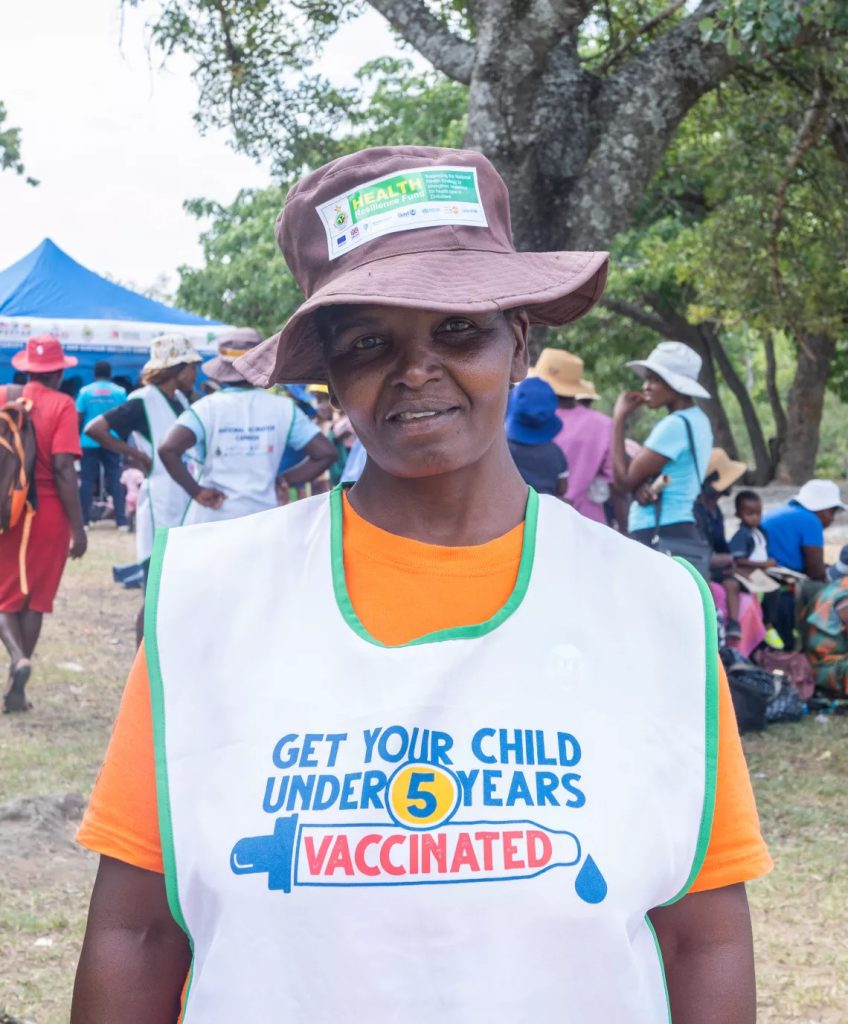
Village Health Workers are vital to linking people in need with health care services. They have the best understanding of the local communities.
They are crucial in mobilising mothers to bring their small children for preventive and curative health services to the local health facilities and outreach activities.
Village Health Workers have been instrumental in reducing the maternal mortality ratio from a peak of 960 in 2010 to 462 per 100,000 live births in 2019 and of the infant and under-five mortality rate from 67 and 94 in 2010 to 47 and 65 per 1,000 live births in 2019.
SOURCE:: unicef.org via link https://www.unicef.org/zimbabwe/stories/matabeleland-south-happy-change-health-resilience-funds-bringing















Recent Comments